40 years ago this month, the International Code of Marketing of Breast-milk Substitutes was adopted by the World Health Assembly. In this four-part series starting today, David Clark, UNICEF’s legal specialist for 25 years until his retirement in December 2020, charts the Code from its beginning, gives us a check-up on where it is today, and helps clarify its path forward.
 David Clark joined UNICEF’s Nutrition Section as the Legal Specialist in 1995, a post he held until December 2020. During his tenure he assisted more than 60 countries in drafting legislation to implement the International Code of Marketing of Breastmilk Substitutes and subsequent resolutions of the World Health Assembly (the Code), and has been instrumental in bringing a human-rights based approach to the protection, promotion and support of breastfeeding.
David Clark joined UNICEF’s Nutrition Section as the Legal Specialist in 1995, a post he held until December 2020. During his tenure he assisted more than 60 countries in drafting legislation to implement the International Code of Marketing of Breastmilk Substitutes and subsequent resolutions of the World Health Assembly (the Code), and has been instrumental in bringing a human-rights based approach to the protection, promotion and support of breastfeeding.
By David Clark

Although it was over 25 years ago, I remember my first day as the UNICEF legal specialist like it was yesterday. I dressed up nicely and carried a brand new leather briefcase (in those days people still carried briefcases). My supervisor dropped by UNICEF’s small nutrition section, briefly welcomed me, showed me my desk and gave me a copy of the International Baby Food Action (IBFAN) Code Handbook, still in draft form. Then she announced she had been called away urgently on a mission and promptly left.
Her exit, if hasty, gave me time to read through the manual thoroughly. On her return she proved to be an invaluable mentor, and soon after, I was sent on a mission myself – to Penang, Malaysia, headquarters at the time of IBFAN’s International Code Documentation Center, to be trained by the experts. And so my Code journey began.
Twenty-five years seem to have gone by quickly – and so have the 40 years since the Code was adopted by the World Health Assembly by a vote of 118-1 in May 1981, the U.S. the lone nay; three countries abstained. But what has changed? In some ways a lot, and yet, in some painful, tragic ways, very little.
A lot: Researchers have published numerous articles, confirming that there really is no substitute for breastmilk. We understand so much more today about breastmilk and its almost dizzying list of benefits – to mother, child, and society at large – and the risks of not breastfeeding. The human rights community now understands breastfeeding as an integral part of a child’s right to survival, health and development.
A little: The breastmilk substitutes (BMS) industry seems to have hardly heard the news. It has only expanded and grown, contributing to untold millions of child deaths and draining valuable economic resources, from families, communities and governments, that could be focused on strengthening health, education and social welfare services and programs to improve maternal, infant and young child nutrition.
As we mark the 40th anniversary, in this series I’ll look at what has gone right and what has gone wrong from the unique position I occupied. But first, I want to be clear what’s at stake – 40 years on, the Code is more important than ever because we know it can stop the BMS companies from using misinformation and deceit to promote their products. A chart from Julie Smith of the Australian National University, published in the Australian Breastfeeding Association’s Essence Magazine in 2016 and based on data from the Euromonitor International Passport Global Market Information Database is our proof.
As these data show, in countries where there is strong Code implementation, the sales of BMS products stagnate; in countries where it is not, the sales increase.
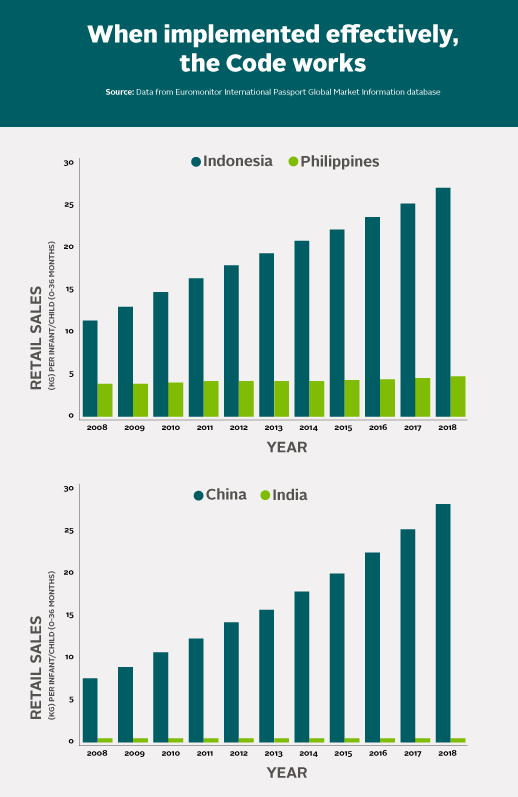
How have India and the Philippines achieved effective implementation of the Code?
In 2008, Euromonitor highlighted that China and Indonesia were the top countries to help drive future sales of baby foods, with toddler milk (a BMS) being the best performing category. Noting that government regulation was a “growing constraint” on sales, the report pointed out specifically that, “In India, all advertising is prohibited, while in China, TV advertising and the use of celebrity spokespeople are allowed.”
India has always been held up as an example of what governments should do. Lawmakers enacted the country’s first Infant Milk Substitutes Act in 1992, and then strengthened it in 2003, banning all forms of promotion of foods marketed to children up to two years of age and sponsorship to health care professionals and associations by the baby food industry.
But the government also took steps to monitor and enforce their law. Violations of the IMS act are considered criminal offenses and may result in fines and imprisonment. Monitoring of the IMS Act is carried out by four NGOs, food safety officials, and other authorized government officials.
Similarly, the Government of the Philippines has shown consistent political will to enforce its 1986 Milk Code, particularly through the adoption of stringent implementing rules and regulations in 2006, and fighting off a challenge by an industry association, the Pharmaceutical and Health Care Association of the Philippines, that included three U.S. formula manufacturers, in the Supreme Court of the Philippines. I was lucky enough to attend the oral arguments in Manilla in July of 2007 and was particularly pleased when the legal representative for industry was forced reluctantly to admit that, indeed, there is no substitute nor replacement for breastmilk.
What’s Law Got to Do With It?
My career at UNICEF began after I saw an announcement seeking a legal specialist, and jumped at the opportunity. I had been working in international development for several years and after working indirectly with a UNICEF project in Myanmar, I was greatly impressed with what they were doing on the ground and knew immediately that I wanted to be part of their 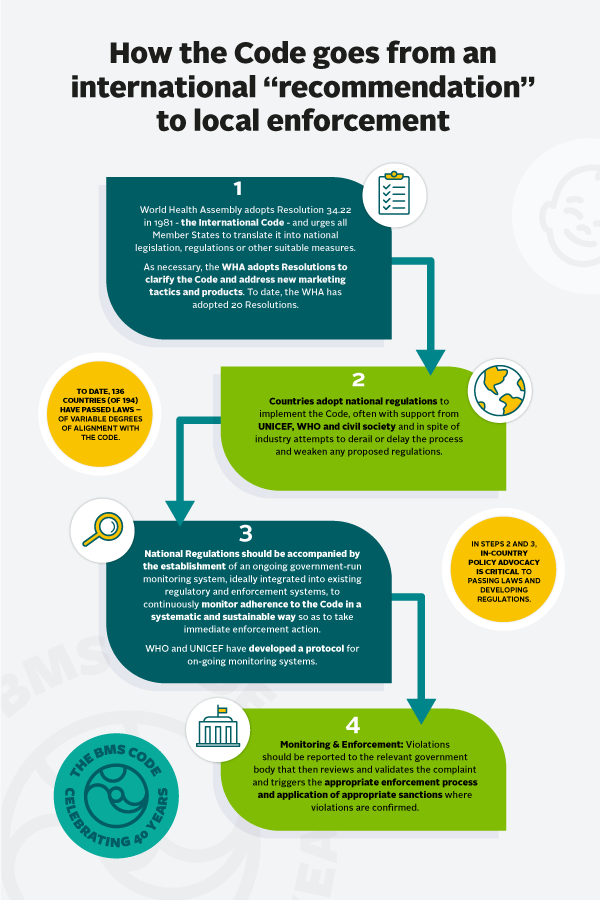 mission. Only later did I realize that the position revolved around the protection of breastfeeding. “What’s law got to do with it?” I asked myself. As it turned out, a great deal.
mission. Only later did I realize that the position revolved around the protection of breastfeeding. “What’s law got to do with it?” I asked myself. As it turned out, a great deal.
For years, the multi-billion-dollar breastmilk substitute industry has spent vast amounts of money aggressively promoting its products. In the process, they mislead and exploit the public, making false claims about their products and deliberately omitting information on the risks associated with their use.
When I started at UNICEF, I had no idea that the immune systems of newborn babies are not fully developed, and the baby is dependent on the immunological properties in her mother’s milk to protect her from illness and infection. This is particularly important in low- and middle-income countries with high rates of infant mortality; but even in high income countries, non-breastfed children get sick more often, require hospitalization and put a financial strain on healthcare systems and families – not to mention the emotional stress for parents and caregivers.
The costs of not breastfeeding are enormous: almost one million children and mothers die annually due to inadequate breastfeeding and the world loses about US $1 billion a day. Explore the data behind these alarming costs.
How many people are aware that, when improperly used, use of BMS (or indeed feeding a newborn anything other than breastmilk) increases the risk of sickness and death? Or that powdered infant formula is not sterile and may contain highly contagious and potentially lethal bacteria and must be prepared with water that is no less than 70 degrees centigrade to reduce the risk of contamination?
There are occasions when BMS products may be necessary – for example in the case of orphaned babies. But they must be used properly and the Code is critical to ensuring that they are prepared safely, through the inclusion of necessary warnings and instructions on labels, and reminding the public that they should only be used on the advice of a health worker.

Parents have a right to know all these facts before deciding how to feed their babies, and the only way to ensure they do is to stop the BMS industry from using their marketing tricks to mislead and manipulate them. Laws are essential to doing exactly that – it’s why the public health community acted 40 years ago to establish the International Code of Marketing of Breast-milk Substitutes.
I am often asked, “What is this International Code?” Is it a treaty or a convention? If a company violates it by, for example, putting up a billboard advertising a BMS or offering a mother a free sample, is there an international body that monitors its implementation and can impose some sort of sanction?
Over the years, many people have contacted me hoping that UNICEF, WHO or some other body has the authority to police and enforce the Code. But unfortunately, that isn’t the case. The Code is a recommendation, albeit from the World Health Assembly, the highest international public health policy-making body, but that effectively means countries must enact laws – and then implement mechanisms to monitor and enforce them to end the promotion of the products that are the subject of those laws (see graphic above). As I explain later in this series, governments that have ratified the Convention on the Rights of the Child (every Government in the world with the exception of the U.S.) are legally bound to implement the Code under international human rights law.

As we mark the Code’s 40th anniversary, we must acknowledge that this takes time and sustained advocacy – particularly because company profits are so immense. They have a lot to lose. So, they’re not going to stop promoting these products without a fight. The history of the Code tells us nothing less.
In Part 2, David looks at the history of the Code.
Return to the Code landing page.
